Ways We Care
You and your child are welcomed by an expert pediatric care team in a warm space where the whole family is respected and supported. You can expect comprehensive pediatric medical services, including mental health and lactation support, expert newborn care, and same-day visits for illness or injury. Learn about all the ways we care for kids.

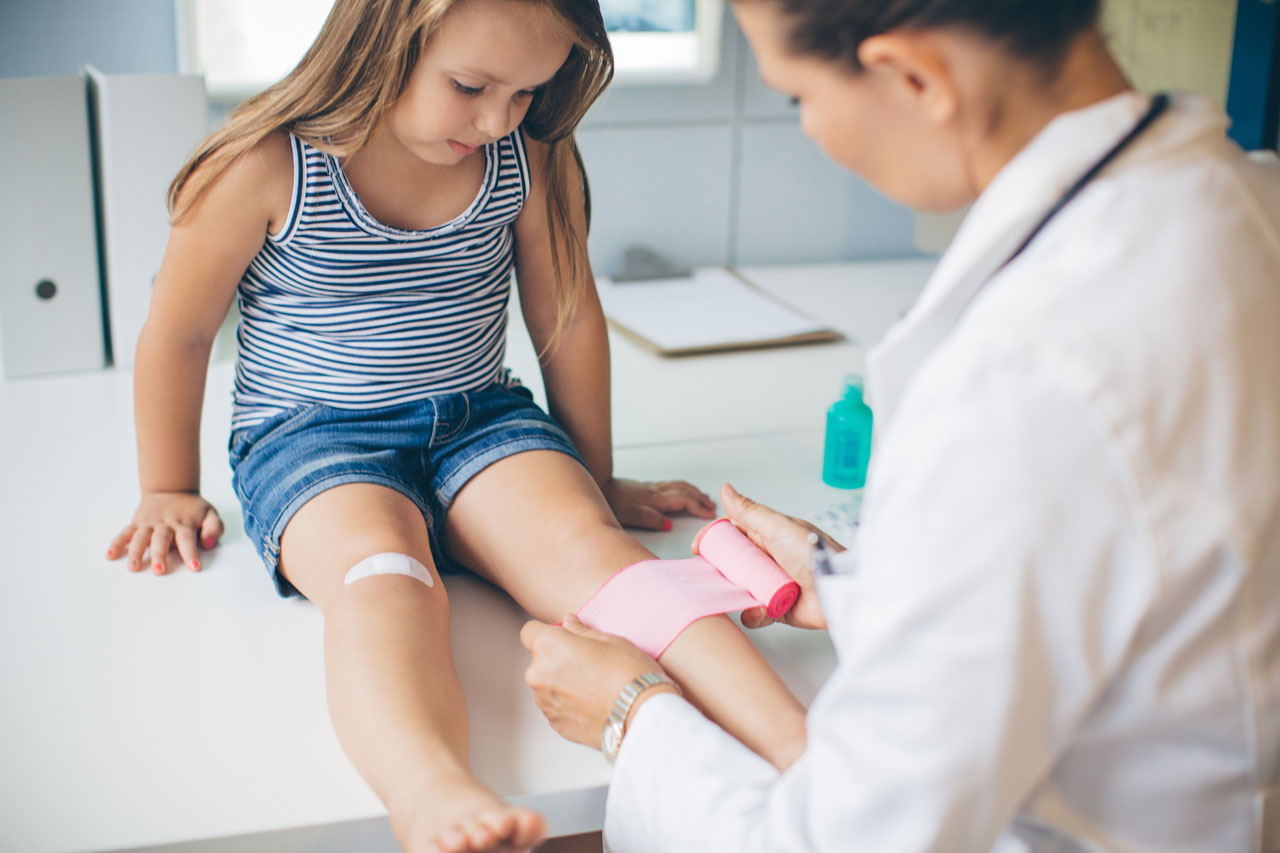
Open Every Day with 24/7 Nurse Advice
Kids don’t get sick on a schedule. That’s why we’re open 7 days a week, offering same-day appointments, plus 24/7 phone nurse advice. With 6 pediatric clinics in the Portland metro area, there’s a location close to you.
Lactation Support
We’re passionate about helping parents and babies succeed at breastfeeding and early nutrition. Metro’s team of certified lactation consultants (IBCLCs) is here to support you with expert nursing guidance for families of all types.

Six Pediatric Clinics in the Portland Metro Area
Choose from pediatric clinics in Portland, Beaverton, Tigard, Happy Valley, and Gresham with over 50 providers to serve kids of all ages.
View All LocationsWhat Our Patients Say About Us
I came in for my baby’s first well check and was almost late, overwhelmed and exhausted. Started crying at the front desk and one of the beautiful ladies walked out to the front and gave me a hug and made me feel SO much better. We also had a wonderful experience with both doctors we’ve seen. We were given in depth answers to every question and felt very comfortable and supported. I am delighted with this clinic, to say the least!!!

Beaverton
I can not say enough about this place. From the moment I called to inquire about their clinic to walking in the door I was completely impressed. The front staff was super friendly. The main entrance is so kid friendly & even fun for adults. The nurses explained everything so clearly & answered all my questions. The exam rooms are so cool! When they built their office they kept kids in mind in every aspect. The Dr was amazing. She made me feel calm & hopeful. I am struggling with sleep training & she gave me several things to try and told me to email or call with any questions or concerns. I haven’t been to a Dr office in a long time where they actually made me feel heard. No rushing. A completely incredible experience, I can’t wait to go back 😉❤

Bridgeport
We have been with Metro for the past 5 years and it has been exceptional. We have had the same doctor the whole time, which means we feel our family is known and our concerns are heard. Even with the challenges the medical world has undergone since 2020, we have felt well supported and very comfortable with the atmosphere at Metro. If only there were clinics for adults as well thought out as Metropolitan pediatrics.

Gresham
Punctual, efficient, personable and friendly –
This was our first appointment since switching from Doernbecher and it’s completely different from what we experienced there for the past 2 years. We already feel at home! Thank you for being so friendly and welcoming 🙂

Johnson Creek
Metropolitan Pediatrics is amazing!! All of the doctors are so wonderful with the kids and extremely knowledgeable!! 🙂
I cant say enough good about the care and personal touch given ~ each time! 🙂

Sunnyside
Really wonderful experience getting my daughter’s ears pierced here! Such friendly and welcoming staff, they made her feel very special for this experience and spoke to her personally, explaining everything in ways that she could understand. 100% recommend for ear piercing by medical professionals!

NW Portland
Parent FAQs
Metropolitan Pediatrics announcements and blog articles with answers to parents’ questions on how to care for kids.
View All FAQs Top Benefits of Saline Nasal Spray for Newborn Care
Top Benefits of Saline Nasal Spray for Newborn Care
Most babies struggle at some point with nasal congestion that interrupts their sleep and feeding patterns, leading to fussiness and... Read More ›
 10 Soft Foods for a Child’s Diet in Illness Recovery
10 Soft Foods for a Child’s Diet in Illness Recovery
It’s never fun for kids to feel sick. Most of us know that it’s important when recovering from an illness... Read More ›
 6 Important Ways That Well-Child Exams Support a Child’s Development
6 Important Ways That Well-Child Exams Support a Child’s Development
Healthcare experts recommend that children see their primary care physician for well-child exams on a schedule outlined by the American... Read More ›
 Understanding Complex Care for a Child with Unique Medical Needs
Understanding Complex Care for a Child with Unique Medical Needs
Some children have unique medical needs including complex conditions that require specialized medical care, treatment, and support. Metropolitan Pediatrics offers... Read More ›
 Pediatric First Aid Basics: What Every Caregiver Should Know
Pediatric First Aid Basics: What Every Caregiver Should Know
The Importance of Pediatric First Aid Medical emergencies are unpredictable. When they involve our children, the emotional toll can spike... Read More ›
 How to Manage Allergies in Children: From Food to Pollen
How to Manage Allergies in Children: From Food to Pollen
The Importance of Understanding Allergies in Children Allergies in children are not just a mere inconvenience; they represent how the... Read More ›
 Most Common Symptoms of an Ear Infection
Most Common Symptoms of an Ear Infection
Ear infections are among the most common ailments where parents bring their child to the doctor. It helps to understand... Read More ›
 Metro Accepts BlueCross BlueShield Health Insurance
Metro Accepts BlueCross BlueShield Health Insurance
Notice to Metro Pediatrics Patients Metro is contracted with BlueCross BlueShield as your in-network provider and welcomes all patients with... Read More ›
 Recognizing and Supporting Mental Health in Children
Recognizing and Supporting Mental Health in Children
The Importance of Mental Health in Children As parents, educators, and caregivers, we work together to ensure the wellbeing of... Read More ›
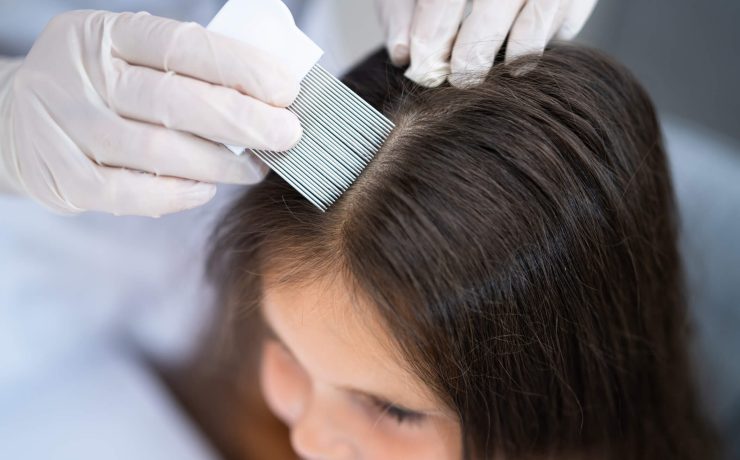 How to Get Rid of Head Lice
How to Get Rid of Head Lice
Head lice. Is it cause for real concern? For some, there’s an “ick” factor associated with a head of lice... Read More ›
 How to Recognize Common Childhood Illnesses
How to Recognize Common Childhood Illnesses
Most every parent can relate to being worried or feeling frantic when trying to understand the best way to care... Read More ›
 10 Ways to Ensure Good Nutrition for Child Development
10 Ways to Ensure Good Nutrition for Child Development
Good nutrition is foundational in the healthy development of a child. Healthy food provides vitamins and minerals, fiber, protein, and... Read More ›













